Dot blot hemorrhages8/13/2023  Also, fibrinoid necrosis of choroidal arterioles occurs leading to segmental infarction of choriocapillaries. Severe intracranial hypertension leads to optic nerve ischemia and edema (papilledema). In this stage, retinal signs occur such as retinal hemorrhage (flame-shaped and dot blot), hard exudate formation, necrosis of smooth muscle cells and retinal ischemia (cotton-wool spots). Seen in patients with severely increased BP characterized by the disruption of the blood-brain barrier and leakage of blood and plasma into the vessel wall disrupting the autoregulatory mechanisms. 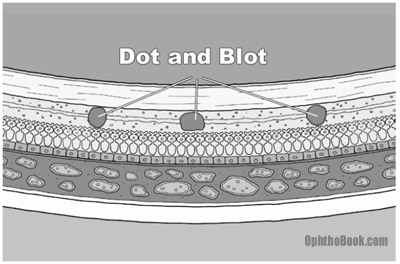
The vein, in turn, appears dilated and torturous distal to the AV crossing. Important aspects of workup regarding diabetic retinopathy include fasting glucose and hemoglobin A1c (HbA1c), fluorescein angiography, optical coherence tomography, and B-scan ultrasonography. AV crossing changes occur when a thickened arteriole crosses over a venule and subsequently compresses it as the vessels share a common adventitious sheath. This leads to a severe form of arteriolar narrowing, arteriovenous (AV) crossing changes, and widening and accentuation of light reflex (silver and copper wiring). It was observed that plasma leptin levels were higher in patients with hypertensive retinopathy and postulated that it is associated with vascular endothelium damage. In subacute or late presentations in which disc swelling has resolved (with or without collateral vessel formation), the flame-shaped hemorrhages clear first, leaving deeper dot/blot hemorrhages that may be difficult to distinguish from a severe microangiopathic retinopathy such as diabetic retinopathy ( Fig. Renal dysfunction (persistent microalbuminuria and low creatinine clearance) in patients has shown to be a marker for hypertensive retinopathy and end-organ damage. Smoking is considered to have a strong association with severe or malignant hypertensive retinopathy as studied by Poulter et al. studied the genetic factors linked to hypertensive retinopathy and found the deletion of the allele of the angiotensin-converting enzyme has a higher risk associated with the development of hypertensive retinopathy. Genetic factors can also play a role with certain genotypes associated with an increased risk of hypertensive retinopathy. Diagnosis is by funduscopy further details are elucidated by color. Symptoms may not develop until late in the disease. The prevalence of hypertensive retinopathy is more in Afro-Caribbean as compared to Europeans and more in women as compared to men. Manifestations of diabetic retinopathy include microaneurysms, intraretinal hemorrhage, exudates, macular edema, macular ischemia, neovascularization, vitreous hemorrhage, and traction retinal detachment. The examiners were blinded to these factors.Apart from essential and secondary hypertension, there are other factors which play an important role in the development of hypertensive retinopathy. Factors assessed before examination included time since delivery, length of labor, method of delivery, use of forceps, gestational age, Apgar scores, birthweight, head circumference, maternal parity, occurrence of episiotomy, maternal analgesic, maternal anesthesia, and induction of labor. Degree or severity of hemorrhage was classified into 3 categories: Grade I, 1 or 2 hemorrhages Grade II, 3–10 hemorrhages and Grade III, 10 or more hemorrhages. Hemorrhages were classified into 3 zones defined by distance from the optic nerve head and fovea, progressing peripherally from Zone I to Zone III. If retinal hemorrhage (RH) was detected, indirect ophthalmoscopy was repeated every 2 weeks until the RHs were no longer evident. 
Infants with known or suspected systemic or ocular disease were excluded from the study and retinal specialists examined all subjects within 30 hours of birth. The authors report a cross-sectional study of 149 newborn babies free of known medical problems admitted to the Well Baby Nursery of the Children’s Hospital of Yale-New Haven Medical Center over a period of 65 weekdays. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
